
For any non-product related queries, please write to info@perfios.com.
For any non-product related queries, please write to info@perfios.com.
● The IRDAI has announced a comprehensive plan to extend insurance access to every Indian by 2047.
● The plan calls for an affordable insurance product (Bima Vistaar) distributed through a workforce of women at the Gram Panchayat Level (Bima Vahak) and serviced by an all-in-one insurance product purchase and claims processing platform (Bima Sugam)
● Insurtech will play a crucial role in scaling up every part of the customer cycle to reach the target insurance penetration.

At the Global Fintech Fest 2023, jointly organized by the NPCI and a number of other government bodies, IRDAI Chairman Debashish Panda said that the time for ‘Insurance 2.0’ has arrived and the insurance sector in India must evolve and reinvent itself. Commending and highlighting some of the initiatives undertaken by IRDAI, Panda outlined the broad goals he envisioned for the insurance sector in the upcoming decades. One of these initiatives is the ‘Bima trinity’, a broad-ranging program aimed at launching and distributing an affordable single policy that covers life, health, property and accident insurance, providing almost instantaneous claims settlement, with value-added services such as gym or yoga memberships at the time of buying a policy.
India’s financial tech stack is ushering in democratized access to credit, payments, savings, investment, and security for 1.2 billion Indians. In the burning light of tech advancement, this simple new insurance product launch might get lost in the glare despite having the potential to be transformative to citizens and insurance carriers alike.
The word Bima derives from the Hindi word for insurance. Trinity refers to the three component programs that comprise this initiative – Bima Sugam, Bima Vahak and Bima Vistaar.
Bima Sugam is an online portal where customers can compare and purchase policies, settle claims, and conduct renewals. The platform would act as a single window for customers and policy holders to access products from multiple insurance companies and to manage their insurance cover. The interface is purportedly equipped to enable paperless claims settlement, be it health coverage or death claims, based on policy numbers alone. Under the structure of Bima Sugam, both life insurance and general insurance companies are slated to possess a 47.5 percent ownership stake each, while brokerages and agent organizations will each own 2.5 percent.
Bima Vahak is a women-centric dedicated insurance distribution channel that is aimed at increasing insurance inclusion and awareness at the village/Gram Panchayat level. The feeder objective to this goal is the identification and development of local resources who understand and appreciate local needs and enjoy the trust and confidence of the local population of their village/Gram Panchayat. Bima Vahak guidelines released by the IRDAI call for deploying these resources before 31st December 2024. Lead insurers of each state/union territory shall coordinate deployment of resources to ensure maximum coverage of Gram Panchayats as per the following structure:
| S. No | Insurer | Gram Panchayats to be covered within the State / Union Territory |
|---|---|---|
| 1 | Lead Life Insurer (s) | 40% |
| 2 | Lead Non-Life Insurer (s) | 40% |
| 3 | Lead Health Insurer (s) | 5% |
| 4 | All other Insurers together | Minimum 15% |
The scope of activities that may be assigned to the Bima Vahaks may include:
i) Filling of proposal forms, KYC requirements through handheld electronic communication devices and issuance of insurance policies.
ii) Coordination and support in policy and claims related servicing, as applicable.
iii) Support in claims settlements
Bima Vistaar is the single insurance product whose distribution and service the other two programs will enable. It will be distinguished by its simplicity. The terms and conditions will be straightforward and easy to understand, ensuring that customers have complete clarity about their coverage. Under the product, the insurer will get coverage of INR 2 lakhs each for life and accident, INR 1 lakh for property insurance and INR 500 per day in the form of Hospicash for hospitalization. To increase coverage, one can buy multiple policies under his/her name. The premium of the policy is likely to range between INR 800-1200 per annum. For comparison, LIC’s Jeevan Umang whole life plan provides a sum assured of INR 2 lakhs costs a 30-year-old insurer a premium of INR 6282 per annum for a 30-year term. This places the bundled policy firmly in the affordable segment for many Indians. Moreover, the product will have simplified terms and conditions to increase comprehension and trust among potential insurers.
Bima Sugam has been hailed by government bodies and insurance industry leaders as a ‘UPI moment’ for insurance, referring to the digital payment system that has revolutionized the way people transact in India. It can be argued that the ‘aha’ moment in insurance occurred already with the advent of insurance platforms and web aggregators like PolicyBazaar. However, leading voices in insurance have said that the existing setup of aggregators is disjointed since each insurance company has its own distribution channels, and that Sugam will hopefully provide consumers access to every single insurance company on its interface. Moreover, the interface is promoted and maintained by regulators, making it a trusted and reputable portal to purchase financial services for a large majority of users that otherwise don’t have faith in or don’t understand web aggregators.

If there is a true UPI moment, it will certainly arise from the expedition of the claims settlement process. On paper, insurers are mandated to settle claims within 30 days of intimation. This time can stretch up to 90 days depending on the need for investigation of the claim. In practice, claims are settled within 10 days of filing. A survey conducted by insurance broker SecureNow placed the average settlement time for health insurance claims between 20 to 46 days. This is inordinately long in an era of instant payments.
Claims processing time isn’t the only problem. The process to file a claim is cumbersome. In life insurance, for example, the claimant must contact the insurance branch office, fill out a claim form, collect a death certificate and other supporting documents and visit the nearest branch office to submit the lot. Bima Sugam aims to cut this process short for life insurance by linking death registries directly to the platform. A policyholder will only need to go to the platform, use their consent to pull their policy and the death certificate. The engine at the back end will process the claim within 6-8 hours. This may also be extended to general insurance with accident records, health records data and property data being digitized by the states on an ongoing basis.
As of today, approximately 500 million people have health insurance coverage in India, accounting for only 37% of the population. Only 3% of the population has some form of life insurance. Clearly, India has a long way to go to provide health and financial protection to all its citizens. However, the upward trend of insurance indicators over the last decade has been encouraging. Total insurance penetration has risen 11.7% between 2020 and 2022, standing at around 4.2% of GDP today, against a global average of 7%. This makes India the tenth largest insurance market in the world growing from $130 billion in 2021 to $420 billion by 2032.
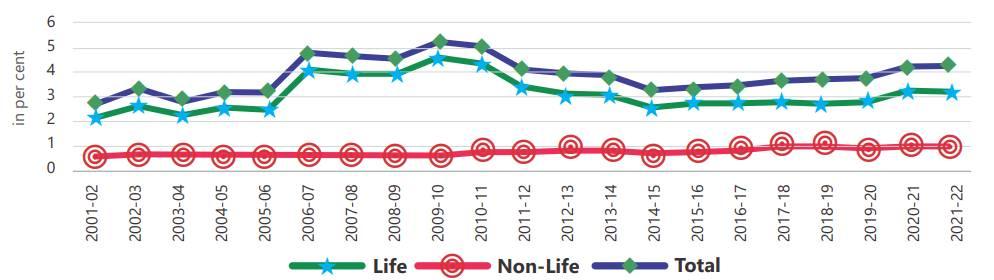
Source: Swiss Re, Sigma, Various issues
The IRDAI has laid out its vision to provide inclusive insurance cover to every Indian citizen by 2047. The focus of IRDAI is to strengthen the three pillars of the entire insurance ecosystem viz. insurance customers (policyholders), insurance providers (insurers) and insurance distributers (intermediaries) by:
1. making the right products available to the right customers.
2. creating a robust grievance redressal mechanism
3. facilitating the ease of doing business in the insurance sector
4. ensuring the regulatory architecture is aligned with market dynamics.
5. boosting innovation, competition and distribution efficiencies while mainstreaming technology and moving towards a principle based regulatory regime.
The Bima trinity is a bold step towards addressing every single one of these ambitions.
The Indian government has launched insurance related schemes in the past targeted at specific use cases. The Pradhan Mantri Fasal Bima Yojana (PMFBY) is a crop insurance scheme launched by the Indian government in 2016, aimed at providing financial support to farmers in the event of crop damage due to natural calamities, pests, and diseases. Under this scheme, farmers pay a nominal premium, and the government provides the remaining premium amount. The coverage is available for all crops and compensation is based on the extent of crop loss. Ayushman Bharat - Pradhan Mantri Jan Arogya Yojana (AB-PMJAY) is an entitlement-based healthcare scheme launched in 2018 and fully funded by the Government of India. AB-PMJAY aims to provide financial protection to over 107million families (approximately 500million individual beneficiaries).
However, Bima Vistaar is the first concerted effort by the government to provide access to an affordable, bundled life and general insurance product.
While the numbers aren’t clear, the Bima Vahak program will potentially provide employment to 2.6 lakh women at the village and Gram Panchayat level. Knowledge of insurance and insurance products will give women in these communities a voice as they interact with their community and share their knowledge. This will play into the critical long-term objective of financial education for all. However, the success of the program is heavily dependent on the regulatory frameworks, training and education provided by insurance companies to their Bima Vahaks. Mis-selling of insurance products is a major industry issue that could be exacerbated by a newly inducted salesforce that may not understand the gravity of the problem. Safeguards against this are yet to be announced by the participating insurance companies.
The Indian government’s vision for insurance penetration entails an overwhelming workload in terms of agent onboarding, KYC, policy underwriting, claims processing and settlement disbursal. It is unlikely that the existing network of TPAs and agency channels will be equipped to scale up to the hours-long turnaround time for claims processing and settlement . Fortunately, Fintech firms have stepped up to the challenge of scaling with proprietary AI and ML-based solutions that can be integrated with insurance carrier systems, government repositories and hospital records repositories.
At Perfios, we provide automation solutions across the business cycle for financial institutions. Our onboarding and verification solutions suites enable one-click onboarding, identity, address and account verification with simple API integration. We have pioneered health claims processing automation with Acclaim - a first of its kind solution that digitizes and categorizes medical claims data allowing almost instantaneous decisioning. Our insurance fraud verification solution, PerSieve, has a proprietary algorithm that flags fraudulent claims information and sorts it into insufficient, unnecessary and excessive treatment categories.
Providing an unprecedented level of claims process digitalization, Perfios is working with multiple domestic and international partners to provide end to end digital customer journeys.
Bima Sugam was slated for launch in January 2023 and has since missed its second deadline, pushed to August 2024. The IRDAI chief has attributed this delay to last minute amendments to the claims settlement and ombudsman process and the eradication of technical glitches. Bima Vahaks are mandated to be deployed by December 31, 2024. And the timelines for Bima Vistaar are yet to be announced.
Whether this trinity is the herald of evolution in the Indian insurance landscape is yet to be gauged.
Perfios Software Solutions is India’s largest SaaS-based B2B fintech software company enabling 900+ Financial institutions to make informed decisions in real-time. Headquartered in Mumbai, India, Perfios specializes in real-time credit decisioning, analytics, onboarding automation, due diligence, monitoring, litigation, automation and more.
Perfios’ core data platform has been built to aggregate and analyze both structured and unstructured data and provide vertical solutions combining both consented and public data for the BFSI space catering to their stringent Scale Performance, Security, and other SLA requirements.
You can write to us at mailto:connect@perfios.com.
For more information on our solutions, contact us at https://solutions.perfios.com/request-for-demo